Forschungsergebnisse der IDEFICS/I.Family-Kohortenstudie
Details zu den Zielen und Methoden sowie wesentliche Ergebnisse der I.Family-Studie aus dem finalen Projektbericht (April 2017) finden sich in englischer Sprache hier. Im Folgenden wurden diese bisherigen Ergebnisse um neuere Forschungsergebnisse aus der IDEFICS/I.Family-Kohorte ergänzt. Listen mit allen Publikationen der IDEFICS-Studie und der I.Family-Studie sind auf den jeweiligen Projekt-Webseiten (siehe oben) unter “Publikationen” bzw. “Projektpublikationen“ zu finden.
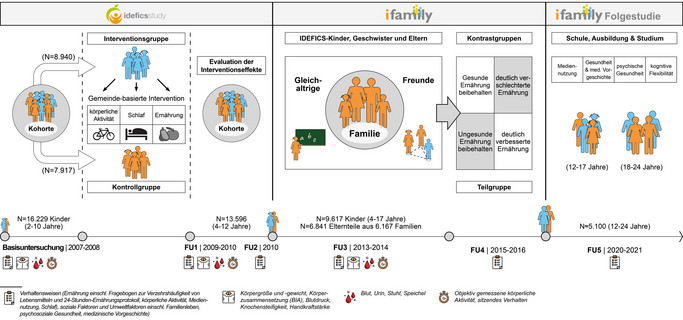
Eine Übersicht über die Erhebungswellen dieser großen europäischen Kohortenstudie mit der Anzahl der Teilnehmenden, den Altersgruppen und den durchgeführten Untersuchungen und Messungen gibt Abbildung 1.
FORSCHUNGSERGEBNISSE
Auswirkung des sozioökonomischen Status auf die Prävalenz/Inzidenz von Übergewicht/Adipositas
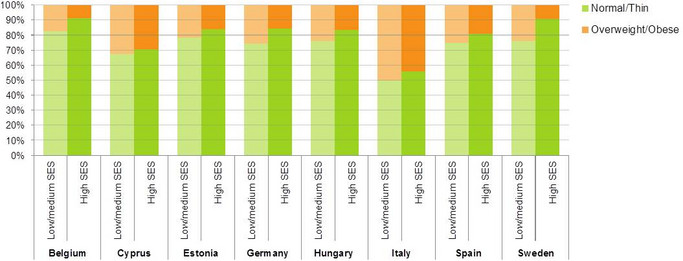
- In den Untersuchungsregionen unterschied sich der Prozentsatz der Kinder mit Übergewicht/Adipositas zwischen Familien mit niedrigerem und höherem sozio-ökonomischen Status (SES), aber auch zwischen den Ländern, wie in Abbildung 2 dargestellt. Hier zeigte sich ein Süd-Nord-Gefälle, wie es auch in anderen Studien beobachtet wurde.
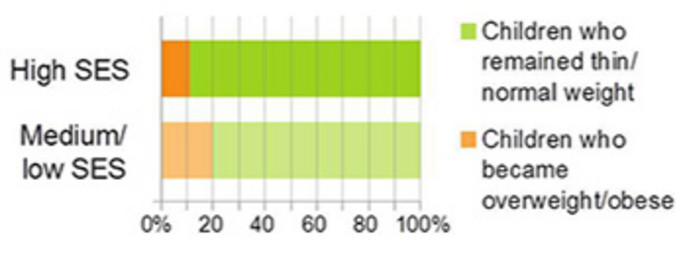
- Je älter die Kinder wurden, desto stärker wurde dieser Effekt. Abbildung 3 zeigt die Inzidenz von Übergewicht/Adipositas nach sozioökonomischem Status (SES) über einen Zeitraum von sechs Jahren. In Familien mit einem mittleren oder niedrigem sozioökonomischen Status (SES) wurden fast doppelt so viele Kinder übergewichtig/adipös wie in Familien mit einem hohen SES.
Ernährung und Kindergesundheit
- Im Durchschnitt aßen die Kinder zu viel energiedichte Lebensmittel, wobei der Verzehr solcher Lebensmittel mit dem Alter zunahm. Die durchschnittliche Energiedichte der von den I.Family-Kindern verzehrten Lebensmittel betrug etwa 2 kcal/g, wobei eine durchschnittliche Energiedichte von etwa 1,25 kcal/g als angemessen angesehen wird. Die Abbildungen 4 und 5 zeigen Beispiele für beliebte Lebensmittel bei europäischen Kindern in Bezug auf die Energiedichte und den Energiegehalt in Kilokalorien.
- Eine gesunde mediterrane Ernährung, die reich an Gemüse, Hülsenfrüchten, Obst, Nüssen, Getreide und Fisch und arm an anderen tierischen Produkten ist, wurde von 30-40 % der Kinder bevorzugt. Bemerkenswert ist, dass dies insbesondere bei schwedischen Kindern der Fall war.1
- Der Zuckerkonsum (alle Mono- und Disaccharide) von Kindern in der I.Family-Studie war sehr hoch und machte teilweise (z. B. in Deutschland) mehr als 30 % der Gesamtenergie aus, unabhängig davon, ob es sich um zugesetzten oder natürlich vorkommenden Zucker handelte. Es zeigte sich, dass die Gesamtzuckeraufnahme sowie der Verzehr von Lebensmitteln und Getränken, die reich an zugesetztem Zucker sind, an Wochenendtagen höher war als an Wochentagen.2
- Kinder, deren Ernährung reich an Gemüse, Vollkorngetreide, Obst und ungesüßter Milch ist und wenig zuckerhaltige Produkte enthält, sind seltener übergewichtig/adipös.3 Nach zwei Jahren war das Risiko, übergewichtig/adipös zu werden, bei Kindern, die sich auf diese Weise ernährten, um 36 % geringer.
- Kinder, die gestillt wurden, wiesen günstige Stoffwechselmarker auf4 und hatten ein geringeres Risiko für Übergewicht in der Kindheit5 (Tabelle 1).
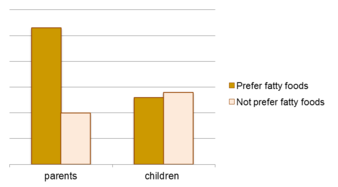
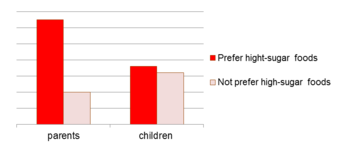
- Eltern, die fettreiche Lebensmittel bevorzugten, konsumierten doppelt so viele fettreiche Produkte wie Eltern, die keine fetthaltigen Lebensmittel bevorzugten. Dies konnte auch bei süßen Lebensmitteln beobachtet werden: Eltern, die süße Lebensmittel bevorzugten, konsumierten dreimal so viele zuckerhaltige Lebensmittel wie Eltern, die keine zuckerhaltigen Lebensmittel bevorzugten. Der Lebensmittelkonsum der Kinder schien jedoch nicht von ihren eigenen Präferenzen beeinflusst zu werden (siehe Abbildung 6).
- Ein ungünstiges Verbraucherverhalten der Eltern, wie z. B. Vertrauen in Werbung oder Nichtvermeidung von Zusatzstoffen, war in allen Ländern mit einer schlechteren Ernährungsqualität der Kinder verbunden.7
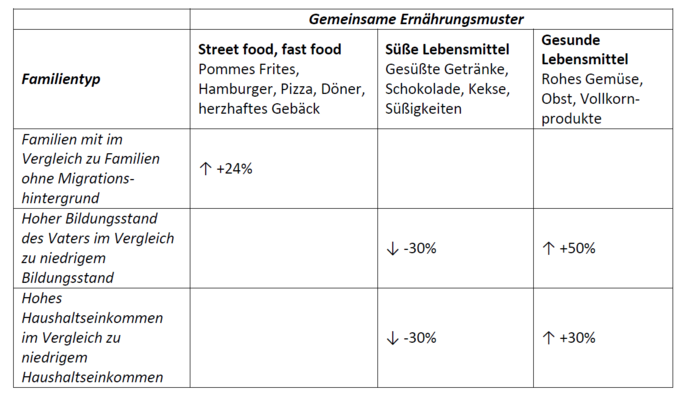
- Die Wahrscheinlichkeit, dass Kinder die gleichen Ernährungsgewohnheiten wie ihre Eltern annehmen ist hoch8, dieser Effekt wird umso stärker, je mehr gemeinsame Mahlzeiten sie einnehmen und ist sogar dreimal so hoch, wenn beide Elternteile die gleichen oder ähnliche Ernährungsgewohnheiten aufweisen.
Mediennutzung
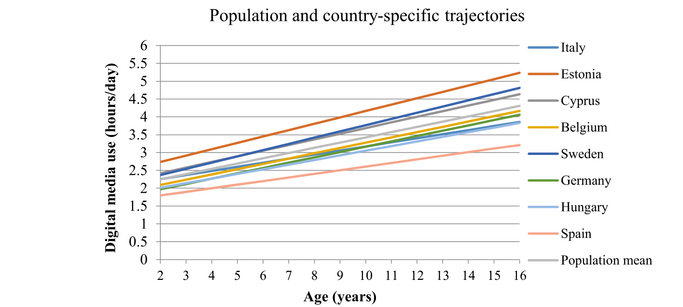
- Digitale Mediennutzung scheint ein Risikofaktor für die Entwicklung von Stoffwechselstörungen bei Kindern und Jugendlichen zu sein. Die mit digitalen Medien verbrachte Zeit nahm mit steigendem Alter der Kinder zu (siehe Abbildung 7). Bei Jungen war der Anstieg mit dem Alter stärker als bei Mädchen und sie wiesen auch ein höheres Risiko für Stoffwechselstörungen auf.
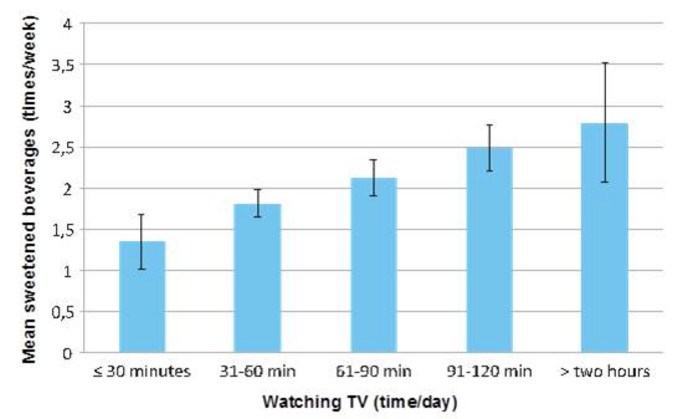
- Eine Teilstudie bei schwedischen Kindern zeigte, dass TV-Werbung ein wichtiger Faktor für den Konsum ungesunder Lebensmittel war. Der Medieneinfluss war bei der Entscheidung, was Kinder essen, tatsächlich stärker als der elterliche Einfluss. Kinder, die länger fernsahen, vor allem Werbefernsehen, tranken viel mehr gesüßte Getränke (siehe Abbildung 8). Dies war unabhängig davon, ob die Eltern diese Getränke ablehnten oder nicht.10
- Kinder, die während des Fernsehens eine Mahlzeit zu sich nahmen, hatten ein um 20 % höheres Risiko fettreiche Lebensmittel zu essen und ein um 30 % höheres Risiko süße Lebensmittel zu essen, als Kinder, die nicht während des Fernsehens aßen. Überraschenderweise war die Wirkung des Fernsehens auf die Kinder gleich, unabhängig davon, ob sie eine starke oder eine geringe Vorliebe für Fett und Süßigkeiten zeigten.11
Schlafmuster – Zusammenhänge mit Ernährung und Gesundheit
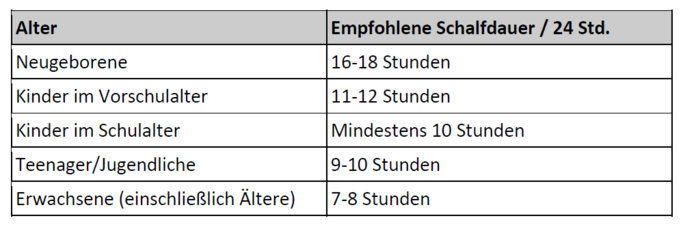
- Nur ein Drittel der Kinder und Jugendlichen erfüllte die vom National Heart, Lung and Blood12 Institute veröffentlichten Empfehlungen zur Schlafdauer (Tabelle 3). Dabei gab es keinen Unterschied zwischen Mädchen und Jungen.
- Kinder, die die Empfehlungen zur nächtlichen Schlafdauer einhielten, aßen mehr Gemüse als Kinder, die die Empfehlung nicht einhielten. Kinder, die die Empfehlungen zur nächtlichen Schlafdauer einhielten, ernährten sich auch insgesamt gesünder als Kinder, die die Empfehlungen nicht einhielten.
- Eine längere Schlafdauer war indirekt, durch ihren günstigen Effekt auf eine abdominale Adipositas, mit einer geringeren Insulinresistenz verbunden. Daher kann sich eine längere Schlafdauer kurz- und langfristig positiv auf den Zuckerstoffwechsel auswirken.13
- Sowohl eine unzureichende Schlafdauer als auch eine schlechte Schlafqualität gingen bei Kindern und Jugendlichen langfristig mit ungünstigen Auswirkungen auf die Knochengesundheit einher.14
Schlaf und Wohlbefinden
- Kinder mit einem schlechten psychosozialen Wohlbefinden (insbesondere emotionale und Verhaltensprobleme, Probleme mit Freunden oder Gleichaltrigen) hatten ein höheres Risiko, übergewichtig zu werden.15
- Übergewichtige Kinder hatten ein höheres Risiko, ein schlechtes psychosoziales Wohlbefinden zu entwickeln – dies betraf insbesondere ein schlechteres emotionales Wohlbefinden, ein geringeres Selbstwertgefühl und Probleme in der Beziehung zu Familie und Freunden.
- Zahlreiche Untersuchungen deuten darauf hin, dass eine kurze Schlafdauer und eine schlechte Schlafqualität das Risiko für Übergewicht bei Kindern erhöhen.16 Unsere Daten unterstützen die Beobachtung, dass Kinder mit niedriger Schlafdauer häufiger übergewichtig sind.17
- Kinder, deren Wohlbefinden sich im Laufe der Zeit verbesserte oder auf einem konstanten Niveau blieb, schliefen nachts tendenziell länger als Kinder, deren Wohlbefinden sich verschlechterte. Außerdem hatten sie in der Regel weniger Schwierigkeiten beim Einschlafen und beim Aufstehen am Morgen.
- Darüber hinaus hatten Kinder, deren nächtliche Schlafdauer sich erhöhte oder konstant blieb, tendenziell ein besseres Wohlbefinden als Kinder, deren Schlafdauer abnahm. Kinder, deren Schlafqualität langfristig gut blieb, hatten tendenziell ein besseres Wohlbefinden als Kinder, deren Schlafqualität sich verschlechterte.
Gutes Wohlbefinden ist entscheidend
- Ein schlechtes Wohlbefinden erhöhte das Risiko für Stoffwechselstörungen indirekt über Verhaltensweisen wie Ernährung, körperliche Aktivität, Schlaf und Mediennutzung sowie über einen höheren abdominalen Fettanteil. Sowohl im Quer- als auch im Längsschnitt zeigte sich, dass ein höheres Wohlbefinden indirekt positive Auswirkungen auf den Blutdruck, den Zuckerstoffwechsel und die Blutfette (Triglyzeride und HDL-Cholesterin) hatte.18
- Ein höheres psychosoziales Wohlbefinden stand mit einer geringeren emotionalen Impulsivität im Zusammenhang, während eine höhere Anzahl belastender Lebensereignisse mit einer höheren emotionalen Impulsivität verbunden war. Daher müssen Wohlbefinden und belastende Lebensereignisse bei der Entwicklung von Gesundheitsförderungsmaßnahmen, die auf eine Verringerung der emotionalen Impulsivität abzielen, stärker berücksichtigt werden.19 Die Verringerung der emotionalen Impulsivität kann zur Vorbeugung von Adipositas beitragen, da Jugendliche mit einer stärkeren Tendenz zur emotionalen Impulsivität angaben, häufiger Snacks zu essen, insbesondere solche mit hohem Energiegehalt.20
Körperliche Aktivität und Kindergesundheit
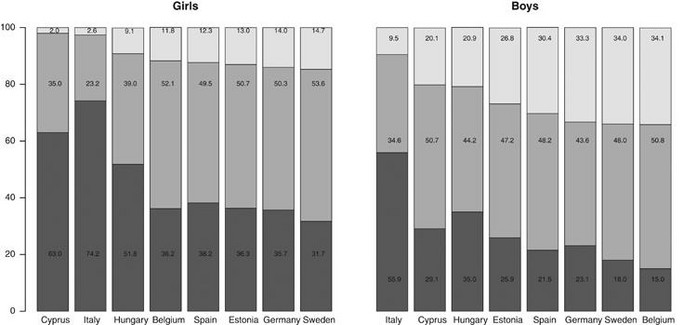
- Nur ein kleiner Anteil der jungen Menschen in unseren 8 europäischen Studienregionen erreichten die aktuellen Empfehlungen für körperliche Aktivität (Box 1), d. h. sie sollten täglich 60 Minuten zumindest mit moderater Intensität aktiv sein (Abbildung 9). Jungen aus Belgien erreichten die Empfehlungen mit dem höchsten Prozentanteil, aber auch von ihnen waren nur 35 % ausreichend aktiv.
- Mädchen waren unabhängig vom Alter weniger körperlich aktiv als Jungen. Die tägliche Dauer der körperlichen Aktivität von Kindern nahm zwischen dem 5. und dem 15. Lebensjahr mit einer durchschnittlichen Rate von 4,3 % ab – die jährliche Abnahme lag bei 4,1% für Jungen und bei 4,5% für Mädchen. Mit zunehmendem Alter verbrachten junge Menschen immer mehr Zeit sitzend. Lag dieser Anteil im Alter von 5-7 Jahren noch bei 40 %, waren es im Alter von 14-16 Jahren bereits 62 % der Zeit, die sitzend verbracht wurde.
- Der Wohnort hatte auch einen Einfluss auf den Geschlechterunterschied in der körperlichen Aktivität. Je nach Land bestanden erhebliche Unterschiede in der Höhe der körperlichen Aktivität. Während die Kinder in unserer italienischen Kohorte am wenigsten aktiv waren, waren die schwedischen Kinder am aktivsten. Der Unterschied in der durchschnittlichen täglichen Aktivitätsdauer zwischen den am wenigsten aktiven Kindern (Italien) und den aktivsten Kindern (Schweden) war größer als der beobachtete Unterschied zwischen Jungen und Mädchen. Tatsächlich waren die Mädchen in den zwei Ländern mit der höchsten körperlichen Aktivität (Belgien und Schweden) aktiver als die Jungen in den Ländern mit der geringsten körperlichen Aktivität (Italien und Zypern).
- Kinder, die die aktuellen Empfehlungen für körperliche Aktivität [60 Minuten moderate bis intensive körperliche Aktivität (MVPA) täglich] erfüllten, hatten im Vergleich zu weniger aktiven Kindern ein geringeres Risiko, im Laufe der Zeit übergewichtig zu werden. Ähnliche Zusammenhänge zeigten sich für täglich 45 min MVPA. Währenddessen war bei Kindern, die im Laufe der Zeit übergewichtig wurden, im Vergleich zu normalgewichtigen Kindern, die Wahrscheinlichkeit am geringsten, täglich 45 oder 60 min MVPA zu erreichen. Demnach ist der Zusammenhang zwischen körperlicher Aktivität und Gewichtsstatus bidirektional.23
- In der gesamten Kohorte gab es einen leichten Trend zu mehr körperlicher Aktivität mit zunehmender Bildung und steigendem Einkommen der Eltern. Dieser Trend war in den acht Ländern ähnlich. Je nach Sozialstatus bestanden einige Unterschiede bei bestimmten Verhaltensweisen (z.B. aktiver Transport, organisierter Sport). Diese waren jedoch bei Betrachtung des Aktivitätsniveaus insgesamt nicht unbedingt zu erkennen.
- Das Ausmaß der körperlichen Aktivität innerhalb der Familie hängt eindeutig zusammen: Aktivere Kinder hatten aktivere Eltern und Geschwister. Diese Beziehung war am stärksten zwischen Geschwistern und nicht ganz so stark zwischen Eltern und Kindern.
- Körperliche Aktivität scheint sich positiv auf die Knochengesundheit auszuwirken. Im Gegemsatz dazu scheint die zunehmend im Sitzen verbrachte Zeit bei Bildschirm-Tätigkeiten ein Risikofaktor für eine ungünstige Entwicklung der Knochengesundheit zu sein, insbesondere bei Kindern und Jugendlichen mit Übergewicht/Adipositas.24
Lokale Umgebung und Bewegungsverhalten
- In dicht besiedelten Gebieten förderte das Vorhandensein von öffentlichen Freiflächen die körperliche Aktivität von Kindern. Hatten die Eltern Sicherheitsbedenken, änderte sich dies jedoch je nach Alter und Geschlecht des Kindes. Wenn Eltern das Gefühl haben, dass die Umgebung für Kinder nicht sicher ist, neigen sie dazu, die Aktivitäten ihrer Kinder im Freien einzuschränken. Dies gilt insbesondere für Mädchen.25
- Für Jugendliche waren insbesondere gute Fuß- und Radwege sowie abwechslungsreiche Ziele wichtig, während öffentliche Freiflächen an Bedeutung verloren. Hinzu kommt, dass die körperliche Aktivität von der Kindheit zum Jugendalter ohnehin stark abnimmt. Unsere Untersuchungen haben gezeigt, dass ein dichtes Wegenetz in Städten diesem Rückgang der körperlichen Aktivität entgegenwirkt, allerdings bestehen Unterschiede zwischen Jungen und Mädchen. Die Anbindung und die Verfügbarkeit von Geh- und Radfahrmöglichkeiten sowie vielfältige Ziele scheinen bei Mädchen einen aktiven Lebensstil im Jugendalter zu fördern, während für Jungen öffentliche Freiflächen ein wichtiger Faktor zur Förderung ausreichender körperlicher Aktivität blieben.
Wie die Familie die Gesundheit von Kindern beeinflusst
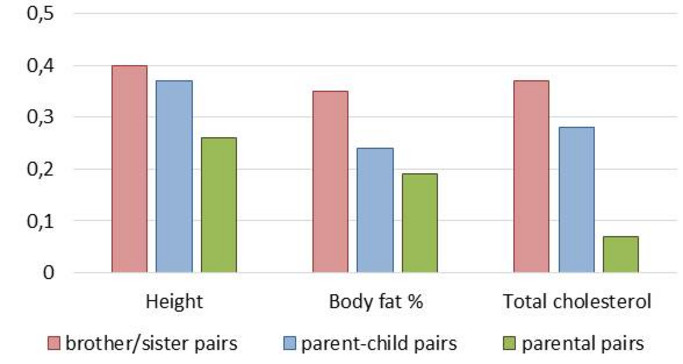
- Familienmitglieder ähnelten sich in Bezug auf Körpergröße, Körperfettanteil und Risiko für Herz-Kreislauf-Erkrankungen (z. B. Gesamtcholesterin) (Abbildung 10).Mütter ähnelten ihren Kindern tendenziell stärker als Väter. Die Ähnlichkeit war bei biologischen Verwandten (Geschwisterpaare, Eltern-Kind-Paare) stärker ausgeprägt als bei nicht-biologischen Verwandten (Elternpaare), was darauf hindeutet, dass diese Merkmale wahrscheinlich einem starken genetischen Einfluss unterliegen. Zwischen Geschwistern bestand hinsichtlich Körperfettanteil und Gesamtcholesterin ein stärkerer Zusammenhang als zwischen Eltern und ihren Kindern, was mit dem gemeinsamen Umfeld der Geschwister zusammenhängen könnte.
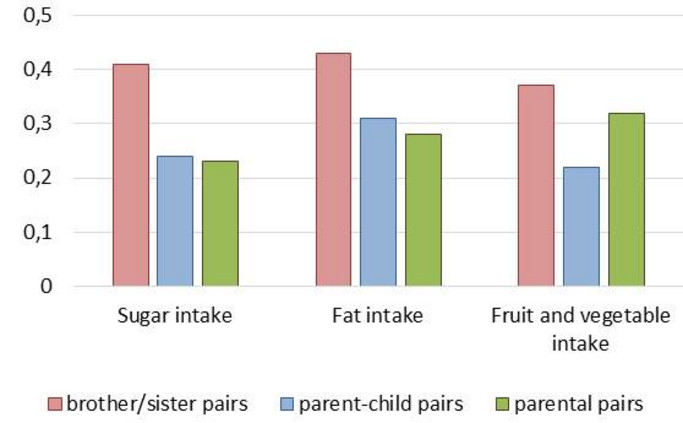
- Familienmitglieder hatten eine ähnliche Ernährungsweise (Abbildung 11). Interessanterweise war die Ähnlichkeit für Geschwisterpaare am größten und die für Eltern-Kind und Eltern-Paare etwas geringer. Da die Ähnlichkeit bei genetisch verwandten und nicht genetisch verwandten Familienmitgliedern ähnlich war, lässt sich schlussfolgern, dass der gemeinsame Haushalt ein wichtiger Faktor für die Ernährungsweise ist.
- Eltern und Kinder hatten ähnliche Muster bei der Lebensmittelaufnahme (Abbildung 12). Dies gilt insbesondere für die Aufnahme gesunder Lebensmittel, weniger jedoch für die Aufnahme ungesunder Lebensmittel. Eine mögliche Erklärung könnte sein, dass es in den entwickelten europäischen Gesellschaften viele äußere Einflüsse gibt, die ungesunde Lebensmittel bei Kindern fördern (z. B. Supermärkte, Werbung, Quengeln der Kinder, damit Eltern ihnen in der Werbung gesehene Produkte kaufen usw.), aber nur wenige äußere Einflüsse für gesunde Lebensmittel.
- Das häusliche Umfeld ist offenbar der wichtigste Faktor für den Verzehr von gesunden Lebensmitteln, einschließlich Obst und Gemüse: Wenn diese Lebensmittel Kindern zu Hause nicht zur Verfügung stehen, ist es mit Ausnahme von Mahlzeiten in Schule oder Kindergarten unwahrscheinlich, dass sie auswärts verzehrt werden.
- Kinder haben von Natur aus eine größere Vorliebe für süße Geschmacksrichtungen als Erwachsene. Daher war es nicht überraschend, dass wir beim Verzehr ungesunder Lebensmittel größere Unterschiede zwischen Kindern und Eltern feststellen konnten.
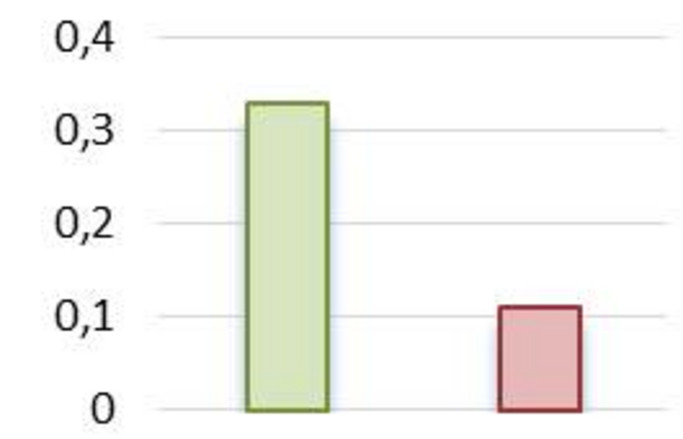
- Familiäre Faktoren erklärten 60 % der Unterschiede bei der Aufnahme gesunder Lebensmittel, aber nur die Hälfte der Unterschiede (30 %) bei der Aufnahme ungesunder Lebensmittel (siehe Abbildung 13).
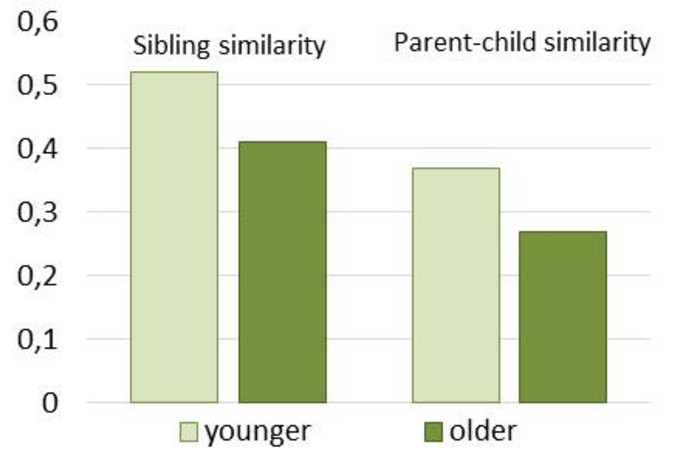
- Hinsichtlich des Verzehrs gesunder Lebensmittel bestand eine größere Ähnlichkeit zwischen jüngeren Geschwisterpaaren (< 11 Jahre) als zwischen älteren Geschwisterpaaren (≥ 11 Jahre) und zwischen Eltern und ihren jüngeren Kindern (< 11 Jahre) als zwischen Eltern und ihren älteren Kindern (≥ 11 Jahre) (Abbildung 14). Dies hängt vermutlich damit zusammen, dass die Häufigkeit der Familienmahlzeiten normalerweise abnimmt und der Einfluss von Freunden an Bedeutung gewinnt, wenn die Kinder älter und unabhängiger werden.
- Bei Geschwister- und Zwillingspaaren, die im selben Haushalt aufwuchsen, stand eine höhere Dauer moderater bis intensiver körperliche Aktivität mit einem niedrigeren BMI im Zusammenhang, während eine höhere Energieaufnahme mit einem höheren BMI verbunden war. Untersuchungen bei Geschwistern erlauben eher Rückschlüsse auf ursächliche Zusammenhänge als solche bei Kindern aus verschiedenen Familien.26
Welchen Einfluss haben Freunde und Gleichaltrige?
- Die Wahrnehmung der Eltern hinsichtlich des Gewichts ihres Kindes wurde davon beeinflusst, wie viel andere Kinder wogen. Die Eltern nahmen ihr Kind als dünner wahr, als es war, wenn die Gleichaltrigen schwerer waren. Ein gegenteiliger Effekt trat auf, wenn die anderen Kinder dünner waren.27
- Der Verzehr ungesunder Lebensmittel von Teenagern stand in engem Zusammenhang mit dem ihrer Freunde (gesüßte Getränke, fettreiche Lebensmittel, zuckerhaltige Lebensmittel, Fast Food). Wir konnten jedoch keinen Zusammenhang beim Verzehr gesunder Lebensmittel unter Gleichaltrigen feststellen (Gemüse-/ Obstkonsum, ballaststoffreiche Lebensmittel).28
- Auch die sitzend verbrachte Zeit und die Bewegungsaktivität in der Freizeit waren bei Jugendlichen und ihren Freunden ähnlich.28
Biomarker und Faktoren, die die metabolische Gesundheit beeinflussen
- Ein hoher Anteil der europäischen Kinder hatte einen Vitamin-D-Mangel. Die im Freien verbrachte Zeit, die Einwirkung von UV-Strahlung und die Vitamin-D-Aufnahme über die Nahrung erwiesen sich als wichtige Faktoren, die den Vitamin-D-Status verbessern können.29
- Die Leptinkonzentration im Blut steht im Zusammenhang mit einer Insulinresistenz (unzureichende Insulinwirkung) und könnte sich bei der Früherkennung von Vorstufen einer Diabetes-Erkrankung als nützlich erweisen.30
- Kinder, die bereits im Kleinkindalter mehrere Stoffwechselstörungen aufweisen, erreichen zumeist auch später im Kindes- oder Jugendalter keinen gesunden Stoffwechselstatus. In diesem Zusammenhang untersuchten wir auch die Rolle von verschiedenen Risikofaktoren bei der Entwicklung von Stoffwechselstörungen von der Kindheit bis zum Jugendalter: Insbesondere weniger elektronische Medien (z. B. Fernseher) im Schlafzimmer, eine Mitgliedschaft im Sportverein und ein besseres Wohlbefinden scheinen die Stoffwechselgesundheit positiv zu beeinflussen.31,32
Rolle von genetischen und epigenetischen Faktoren
- Die Ergebnisse einer Pilotstudie an einer Teilstichprobe der I.Family-Kohorte zeigten, dass eine Reihe zirkulierender microRNAs bei Kindern mit Übergewicht/Adipositas im Vergleich zu Kindern mit Normalgewicht unterschiedlich reguliert waren.33
- Die genetische Veranlagung für die Stoffwechselstörung „Metabolisches Syndrom“ wird weitgehend von Genen für Adipositas (FTO) und für den Fettstoffwechsel (CETP) bestimmt. Daher könnte sich die Einbeziehung der assoziierten Genvarianten in genetische Risiko-Scores für das Metabolische Syndrom als entscheidend erweisen, um Kinder und spätere Erwachsene mit hohem Risiko zu identifizieren, damit früher gezielte Interventionen ermöglicht werden.34
REFERENZEN
- Tognon G, Hebestreit A, Lanfer A, Moreno LA, Pala V, Siani A, Tornaritis M, De Henauw S, Veidebaum T, Molnar D, Ahrens W, Lissner L. Mediterranean diet, overweight and body composition in children from eight European countries: cross-sectional and prospective results from the IDEFICS study. Nutr Metab Cardiovasc Dis. 2014;24(2):205-213.
- Svensson A, Larsson C, Eiben G, Lanfer A, Pala V, Hebestreit A, Huybrechts I, Fernandez-Alvira JM, Russo P, Koni AC, De Henauw S, Veidebaum T, Molnar D, Lissner L, consortium I. European children's sugar intake on weekdays versus weekends: the IDEFICS study. Eur J Clin Nutr. 2014;68(7):822-828.
- Pala V, Lissner L, Hebestreit A, Lanfer A, Sieri S, Siani A, Huybrechts I, Kambek L, Molnar D, Tornaritis M, Moreno L, Ahrens W, Krogh V. Dietary patterns and longitudinal change in body mass in European children: a follow-up study on the IDEFICS multicenter cohort. Eur J Clin Nutr. 2013;67(10):1042-1049.
- Priego T, Sanchez J, Pico C, Ahrens W, Bammann K, De Henauw S, Fraterman A, Iacoviello L, Lissner L, Molnar D, Moreno LA, Siani A, Tornaritis M, Veidebaum T, Palou A, Consortium I. Influence of breastfeeding on blood-cell transcript-based biomarkers of health in children. 10.1111/j.2047-6310.2013.00204.x doi. Pediatr Obes. 2014;9(6):463-470.
- Hunsberger M, Lanfer A, Reeske A, Veidebaum T, Russo P, Hadjigeorgiou C, Moreno LA, Molnar D, de HS, Lissner L, Eiben G. Infant feeding practices and prevalence of obesity in eight European countries - the IDEFICS study. S1368980012003850 pii ;10.1017/S1368980012003850 doi. Public Health Nutr. 2012:1-9.
- Fernandez-Alvira JM, Bornhorst C, Bammann K, Gwozdz W, Krogh V, Hebestreit A, Barba G, Reisch L, Eiben G, Iglesia I, Veidebaum T, Kourides YA, Kovacs E, Huybrechts I, Pigeot I, Moreno LA. Prospective associations between socio-economic status and dietary patterns in European children: the Identification and Prevention of Dietary- and Lifestyle-induced Health Effects in Children and Infants (IDEFICS) Study. S0007114514003663 pii ;10.1017/S0007114514003663 doi. Br J Nutr. 2015;113(3):517-525.
- Jilani H, Pohlabeln H, Buchecker K, Gwozdz W, De Henauw S, Eiben G, Molnar D, Moreno Aznar LA, Pala V, Reisch L, Russo P, Veidebaum T, Ahrens W, Hebestreit A, Consortium) obotIF. Association between parental consumer attitudes with their children’s sensory taste preferences as well as their food choice. PLoS One. 2018;1(13(8):e0200413)
- Hebestreit A, Intemann T, Siani A, De Henauw S, Eiben G, Kourides YA, Kovacs E, Moreno LA, Veidebaum T, Krogh V, Pala V, Bogl LH, Hunsberger M, Boernhorst C, Pigeot I, Consortium IF. Dietary Patterns of European Children and Their Parents in Association with Family Food Environment: Results from the I.Family Study. Nutrients. 2017;9(2):17.
- Sina E, Buck C, Veidebaum T, Siani A, Reisch L, Pohlabeln H, Pala V, Moreno LA, Molnar D, Lissner L, Kourides Y, De Henauw S, Eiben G, Ahrens W, Hebestreit A. Media use trajectories and risk of metabolic syndrome in European children and adolescents: the IDEFICS/I.Family cohort. Int J Behav Nutr Phys Act. 2021;18(1):134.
- Olafsdottir S, Eiben G, Prell H, Hense S, Lissner L, Marild S, Reisch L, Berg C. Young children's screen habits are associated with consumption of sweetened beverages independently of parental norms. 10.1007/s00038-013-0473-2 doi. Int J Public Health. 2014;59(1):67-75.
- Lissner L, Lanfer A, Gwozdz W, Olafsdottir S, Eiben G, Moreno LA, Santaliestra-Pasias AM, Kovacs E, Barba G, Loit HM, Kourides Y, Pala V, Pohlabeln H, de HS, Buchecker K, Ahrens W, Reisch L. Television habits in relation to overweight, diet and taste preferences in European children: the IDEFICS study. 10.1007/s10654-012-9718-2 doi. Eur J Epidemiol 2012;27(9):705-715.
- National Heart L, and Blood Institute. How much sleep is enough? Updated 24.03.2022. Accessed 20.07.2022, https://www.nhlbi.nih.gov/health/sleep/how-much-sleep
- Thumann BF, Michels N, Felso R, Hunsberger M, Kaprio J, Moreno LA, Siani A, Tornaritis M, Veidebaum T, De Henauw S, Ahrens W, Bornhorst C, Idefics, Consortia IF. Associations between sleep duration and insulin resistance in European children and adolescents considering the mediating role of abdominal obesity. PLoS One. 2020;15(6):e0235049.
- Cheng L, Pohlabeln H, Ahrens W, Russo P, Veidebaum T, Hadjigeorgiou C, Molnar D, Hunsberger M, De Henauw S, Moreno LA, Hebestreit A, Idefics, consortia IF. Cross-sectional and longitudinal associations between sleep duration, sleep quality, and bone stiffness in European children and adolescents. Osteoporos Int. 2021;32(5):853-863.
- Hunsberger M, Lehtinen-Jacks S, Mehlig K, Gwozdz W, Russo P, Michels N, Bammann K, Pigeot I, Fernandez-Alvira JM, Thumann BF, Molnar D, Veidebaum T, Hadjigeorgiou C, Lissner L, Consortium I. Bidirectional associations between psychosocial well-being and body mass index in European children: longitudinal findings from the IDEFICS study. BMC Public Health. 2016;16:949.
- Chen X, Beydoun MA, Wang Y. Is sleep duration associated with childhood obesity? A systematic review and meta-analysis. Obesity (Silver Spring). 2008;16(2):265-274.
- Hense S, Pohlabeln H, de HS, Eiben G, Molnar D, Moreno LA, Barba G, Hadjigeorgiou C, Veidebaum T, Ahrens W. Sleep duration and overweight in European children: is the association modified by geographic region? Sleep. 2011;34(7):885-890.
- Thumann BF, Börnhorst C, Ahrens W, Arvidsson L, Gwozdz W, Iguacel I, Mårild S, Molnár D, Rach S, Russo P, Tornaritis M, Veidebaum T, De Henauw S, Michels N. Cross-Sectional and Longitudinal Associations Between Psychosocial Well-Being and Cardiometabolic Markers in European Children and Adolescents. Psychosom Med. 2020;82(8):764-773.
- Do S, Coumans JMJ, Bornhorst C, Pohlabeln H, Reisch LA, Danner UN, Russo P, Veidebaum T, Tornaritis M, Molnar D, Hunsberger M, De Henauw S, Moreno LA, Ahrens W, Hebestreit A. Associations Between Psychosocial Well-Being, Stressful Life Events and Emotion-Driven Impulsiveness in European Adolescents. J Youth Adolesc. 2021;
- Coumans JMJ, Danner UN, Ahrens W, Hebestreit A, Intemann T, Kourides YA, Lissner L, Michels N, Moreno LA, Russo P, Stomfai S, Veidebaum T, Adan RAH. The association of emotion-driven impulsiveness, cognitive inflexibility and decision-making with weight status in European adolescents. Int J Obes (Lond). 2018;42(4):655-661.
- World Health Organization. Physical Activity. https://www.who.int/news-room/fact-sheets/detail/physical-activity
- Konstabel K, Veidebaum T, Verbesterl V, Moreno LA, Bammann K, Tornaritis M, Eiben G, Molnár D, Siani A, Sprengeler O, Wirsik N, Ahrens W, Pitsiladis Y. Objectively measured physical activity in European children: the IDEFICS study Int J Obes. 2014;38(Suppl 2):S 135-S 143.
- Sprengeler O, Pohlabeln H, Bammann K, Buck C, Lauria F, Verbestel V, Eiben G, Konstabel K, Molnar D, Moreno LA, Pitsiladis Y, Page A, Reisch L, Tornaritis M, Ahrens W. Trajectories of objectively measured physical activity and childhood overweight: longitudinal analysis of the IDEFICS/I.Family cohort. Int J Behav Nutr Phys Act. 2021;18(1):103.
- Cheng L, Pohlabeln H, Ahrens W, Lauria F, Veidebaum T, Chadjigeorgiou C, Molnár D, Eiben G, Michels N, Moreno LA, Page AS, Pitsiladis Y, Hebestreit A. Cross-sectional and longitudinal associations between physical activity, sedentary behaviour and bone stiffness index across weight status in European children and adolescents. Int J Behav Nutr Phys Act. 2020;17(1):54.
- Buck C, Tkaczick T, Pitsiladis Y, De Bourdehaudhuij I, Reisch L, Ahrens W, Pigeot I. Objective measures of the built environment and physical activity in children: from walkability to moveability. J Urban Health. 2015;92(1):24-38.
- Bogl LH, Mehlig K, Intemann T, Masip G, Keski-Rahkonen A, Russo P, Michels N, Reisch L, Pala V, Johnson L, Molnar D, Tornaritis M, Veidebaum T, Moreno LA, Ahrens W, Lissner L, Kaprio J, Hebestreit A. A within-sibling pair analysis of lifestyle behaviours and BMI zscore in the multi-centre I.Family study. Nutr Metab Cardiovasc Dis. 2019;
- Gwozdz W, Sousa-Poza A, Reisch LA, Bammann K, Eiben G, Kourides Y, Kovacs E, Lauria F, Konstabel K, Santaliestra-Pasias AM, Vyncke K, Pigeot I. Peer effects on obesity in a sample of European children. Econ Hum Biol. 2015;18:139-152.
- Gwozdz W, Nie P, Sousa-Poza A, DeHenauw S, Felső R, Hebestreit A, Iguacel I, Lissner L, Lauria F, Page A, Reisch LA, Tornaritis M, Veidebaum T, Williams G, Foraita R, Consortium obotIF. Peer Effects on Weight Status, Dietary Behaviour and Physical Activity among Adolescents in Europe: Findings from the I.Family Study. Kyklos. 2019;72(2):270-296.
- Wolters M, Intemann T, Russo P, Moreno LA, Molnar D, Veidebaum T, Tornaritis M, De Henauw S, Eiben G, Ahrens W, Floegel A. 25-Hydroxyvitamin D reference percentiles and the role of their determinants among European children and adolescents. Eur J Clin Nutr. 2021;
- Nagrani R, Foraita R, Wolters M, De Henauw S, Marild S, Molnar D, Moreno LA, Russo P, Tornaritis M, Veidebaum T, Ahrens W, Marron M, Idefics, consortia IF. Longitudinal association of inflammatory markers with markers of glycaemia and insulin resistance in European children. Diabetes Metab Res Rev. 2022;38(3):e3511.
- Börnhorst C. Metabolic status in children and its transitions during childhood and adolescence - The IDEFICS/I.Family study. Int J Epidemiol. 2019;
- Börnhorst C, Russo P, Veidebaum T, Tornaritis M, Molnar D, Lissner L, Marild S, De Henauw S, Moreno LA, Floegel A, Ahrens W, Wolters M. The role of lifestyle and non-modifiable risk factors in the development of metabolic disturbances from childhood to adolescence. Int J Obes (Lond). 2020;
- Iacomino G, Russo P, Stillitano I, Lauria F, Marena P, Ahrens W, De Luca P, Siani A. Circulating microRNAs are deregulated in overweight/obese children: preliminary results of the I.Family study. Genes Nutr. 2016;11:7.
- Nagrani R, Foraita R, Gianfagna F, Iacoviello L, Marild S, Michels N, Molnar D, Moreno L, Russo P, Veidebaum T, Ahrens W, Marron M. Common genetic variation in obesity, lipid transfer genes and risk of Metabolic Syndrome: Results from IDEFICS/I.Family study and meta-analysis. Sci Rep. 2020;10(1):7189.
Offizielle Projekt-Webseiten:
www.ideficsstudy.eu und www.ifamilystudy.eu
Kontakt:
i.family(at)leibniz-bips.de